CT scan information for Health Professionals
Everything you need to know about our low-dose CT service at Mount Vernon.
CT scanning overview
We’ve been offering a CT service since 1985 when our founder, the oncologist Dr Paul Strickland (at the time the medical director of Mount Vernon Cancer Centre) successfully raised funds to buy a CT scanner for Mount Vernon Hospital.
Over the years we have built up considerable expertise in this area and in 2016 scanned more than 6,200 patients per year. We pride ourselves on our fast turnaround times. What sets our service apart is the quality of scans we’re able to produce using our up to date scanner, combined with the expertise of our team.
We have a number of clinical trials running at the centre which require CT scanning techniques and expertise in research reporting.
Why choose us
Our expert team has considerable expertise in CT imaging, using one of the highest resolution CT scanners available today, providing high-quality CT imaging at very low doses for our patients.
The team
Lead Consultant
Our experienced lead consultant and caring radiographers have the specialist training and knowledge required to perform CT scanning techniques safely to the highest standard. The centre fully supports staff through Continuous Professional Development (CPD) – the systematic updating and enhancement of skills, knowledge and competence throughout their career. This includes attendance at external study days, in-house lectures/presentations and Post Graduate Education to MSc level. All radiographers are trained in intra-venous cannulation.
Our lead consultant for CT is Dr Andrew Gogbashian MB BS MRCS FRCR, Consultant Oncological Radiologist.
Dr Gogbashian graduated from Imperial College School of Medicine and is a Consultant Oncological Radiologist and Lead for CT at The Paul Strickland Scanner Centre, Mount Vernon Cancer Centre.
He was a Research Fellow at The Brigham & Women’s Hospital, Harvard Medical School, Boston, USA and is the author or co-author of several peer-reviewed papers, review articles and published abstracts. He has been awarded prizes by the European Congress of Radiology (ECR) and Radiological Society of North America (RSNA).
Dr Gogbashian has an established reputation in oncological imaging with expertise in a range of cancer and non-cancer pathology including low-dose CT scanning, dual-energy CT, multiparametric imaging and whole-body MRI.
Interestingly, his scanning expertise has also been called upon by famous international museums that require high quality CT scans for their precious collections or excavations.
Our CT Scanner
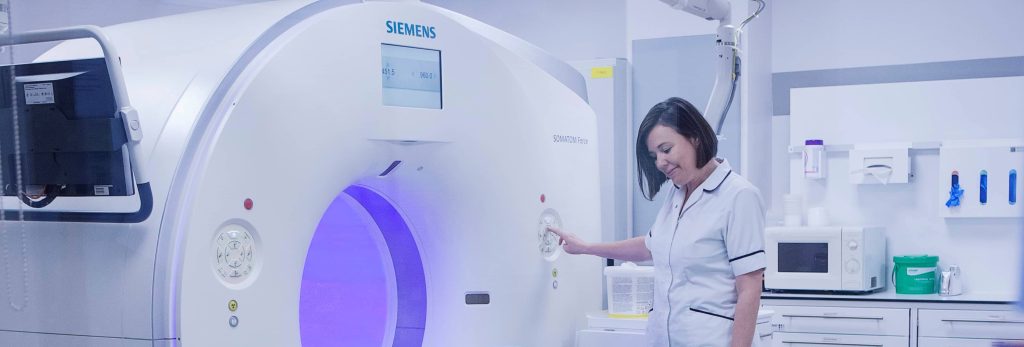
Our current CT Scanner is the Siemens SOMATOM®Force Dual-Energy CT Scanner
The Siemens Force CT scanner, successfully installed at The Paul Strickland Scanner Centre in 2016 as part of our ongoing Scanner replacement programme, is a truly remarkable machine providing many features never seen on CT scanners before.
Its design is extremely suitable for both oncological and non-oncological imaging.
It is one of the highest resolution CT scanners available today, providing high quality CT imaging, at very low doses for our patients.
We are one of the few centres in the UK or worldwide using dual-energy CT imaging as a routine clinical tool for many of our patients. Dual energy CT imaging provides us with the clinical possibility of analysing and characterising tissues with greater detail and accuracy, without compromising dose to patients.
Low dose scanning
The Siemens FORCE CT scanner allows the possibility of reducing radiation dose to patients to unprecedented levels. Using new iterative reconstructiontechniques, we can lower dose without compromising image noise or quality.
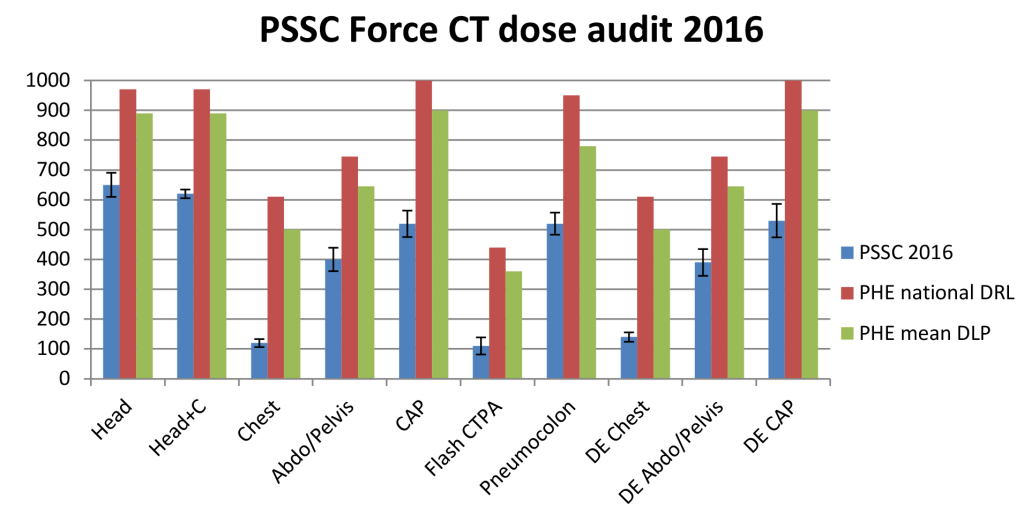
A recent dose audit of a range of CT scans performed at The Paul Strickland Scanner Centre has shown that our CT scan doses are well below National Reference limits.
More detail on the Paul Strickland Scanner Center CT dose audit 2016
Duel energy CT scanning
We are one of the few centres in the UK using dual-energy CT imaging as a routine clinical tool in body imaging. Dual-energy CT uses two x-ray tubes instead of the conventional one x-ray tube to interrogate the body tissues. This allows a more detailed assessment, which can help characterise materials in a new way. The Siemens Force Scanner provides this further detail without compromising on radiation dose as dual-energy CT on this machine is considered “dose neutral”
Example scan images
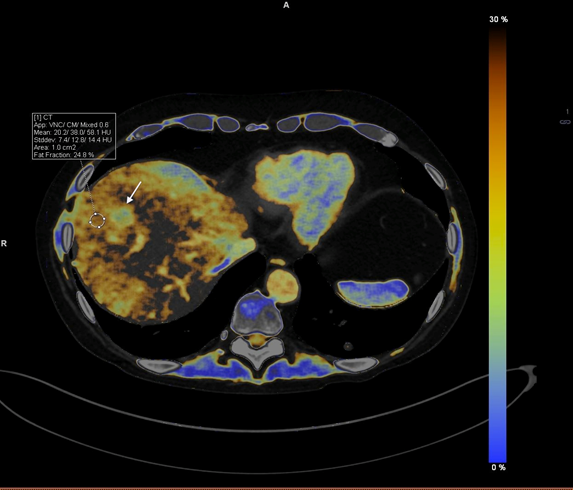
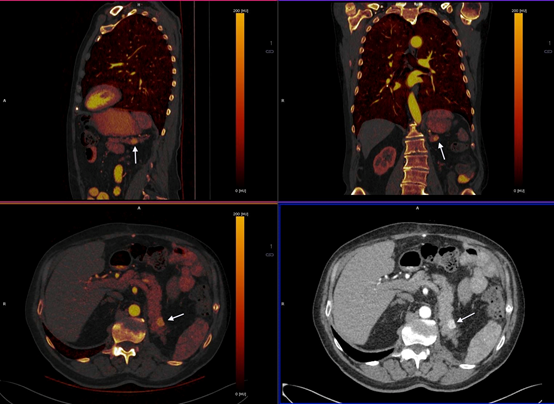
Figure 1B
A fat fraction map of the liver has been obtained utilizing DECT. The background fat percentage of the liver adjacent to the metastasis is 24%. The metastasis is highlighted as a different color due to there being no fat present within the metastasis (arrow) thereby aiding lesion detection.
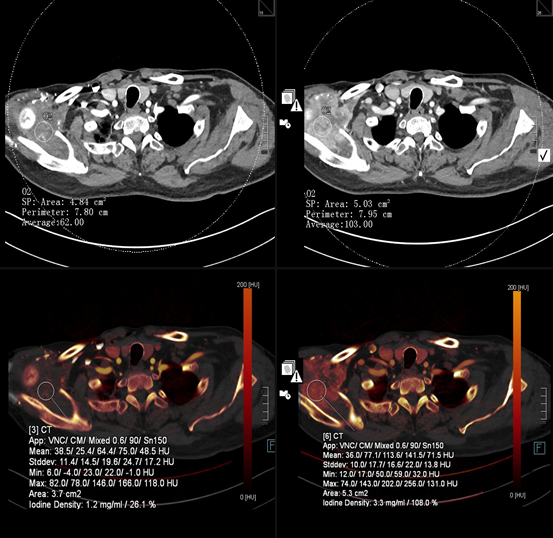
Figure 2
The images on the right demonstrate a large hypervascular renal cell carcinoma metastasis related to the right scapula with extraosseous disease. The images on the left demonstrate the metastasis post 3 months of anti-angiogenic treatment.
The Hounsfield unit (HU) is reduced from 103 to 62 (indicating a therapeutic response by Choi criteria). The iodine maps generated from DECT also demonstrate a therapeutic response by a reduction in iodine density from 3.3mg/ml to 1.2mg/ml. There is a larger percentage reduction in iodine concentration than HU alone (63.6% vs. 39.8%). Change in iodine density can be a more accurate method for assessing therapeutic response due to the exclusion of hemorrhage or other compounding factors, which may affect the assessment.
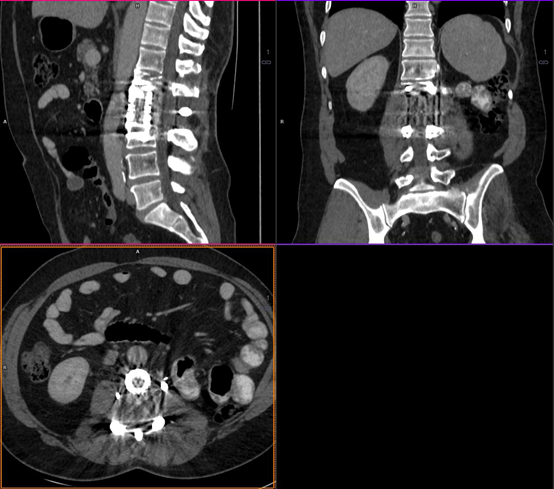
Figure 4A
a) A patient imaged post spinal decompression for metastatic renal cell carcinoma using conventional single-source CT imaging. There is extensive streak artifact across the spinal canal due to metalwork making interpretation of this region problematic in assessing potential relapsed disease.
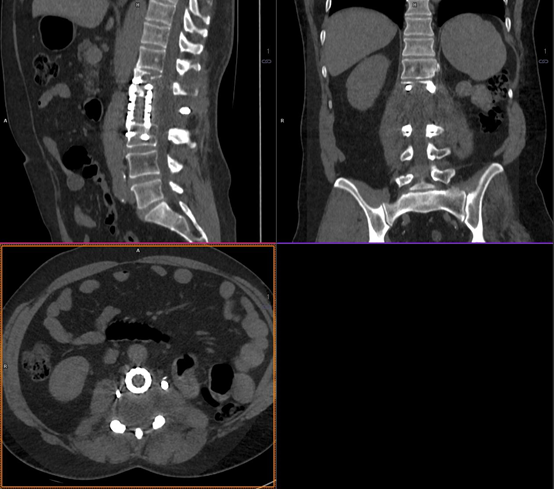
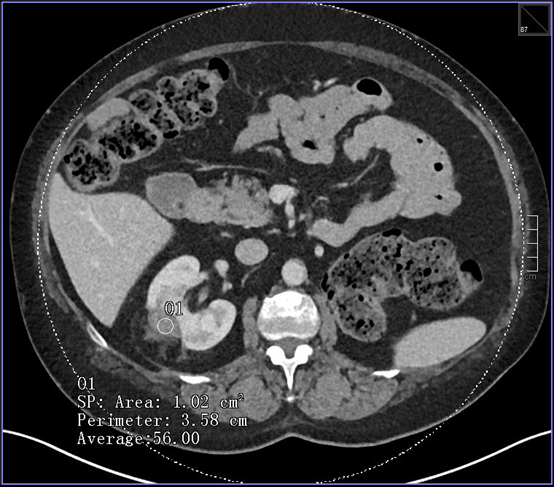
Figure 5A
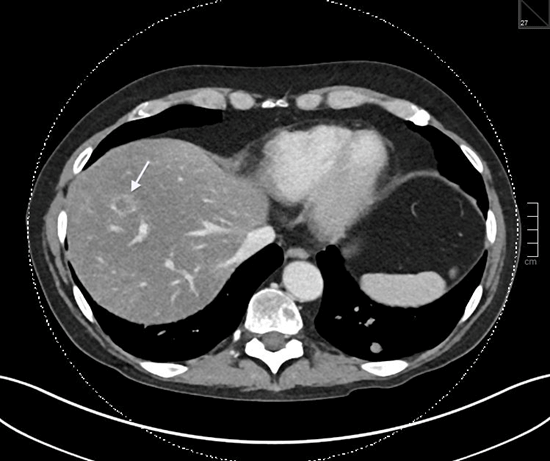
A focus at the midpole of the right kidney with an average HU of 56, 9 months following radiofrequency (RF) ablation for renal cell carcinoma. It is challenging on this CT image alone to determine whether this represents a soft-tissue recurrence or post RF ablation changes which may also be dense.
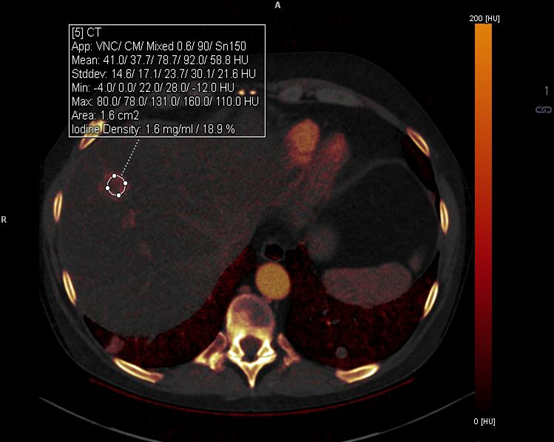
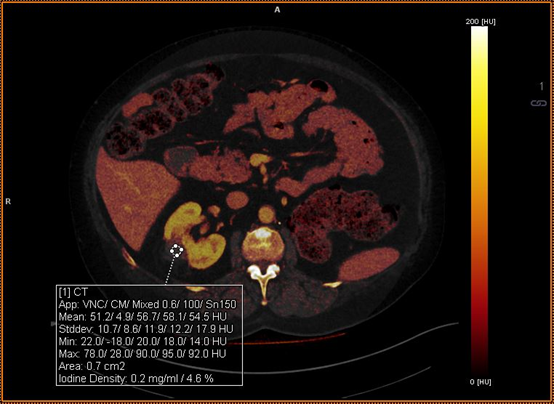
Figure 5B
The same focus at the midpole of the right kidney analyzed with an iodine map generated from DECT. The focus shows virtually no iodine uptake or enhancement, with a mean iodine uptake of 0.2mg/ml (allowing for partial voluming from the adjacent renal cortex) indicating no soft tissue recurrence.